RINOPLASTY
General information
Rhinoplasty is a surgical operation that changes the shape and size of the nose in order to make the face most proportionate and harmonic. No visible scars are left as all of them are located inside the nostrils. In case of breathing difficulties due to a deviated septum or turbinate hypertrophy, these defects can be corrected by means of a septoplasty and/or turbinoplasty in association with a rhinoplasty. Rhinoplasty is a painless operation.
When it is recommended
Rhinoplasty is recommended when the shape and dimensions of the nose create psychological discomfort to the patient or when a previous trauma or surgery altered its shape and/or respiratory function. There are no age limits to undergo a rhinoplasty; however bone and cartilagineous structures of the nose must have reached full development; in adults it will be their general conditions to determine whether they are suitable candidates for this type of surgery or not.
Results
The result is satisfactory from the early days but may appear initially altered due to swelling and bruising. While bruising heals within about ten days, swelling, skin sensitivity, and mobility of the nose take longer, depending on the patient and on the type of surgical procedure performed (even longer for open Rhinoplasty). Complete recovery will take approx. 4 to 6 months and sometimes longer.
Pre-operative preparation
Prior to surgery, the patient must inform the surgeon of any treatment with medications and will have to give up taking acetylsalicylic acid-based medications (aspirin, and products alike). Smoking should be discontinued or at least sharply reduced at least one week prior to surgery. It is necessary to inform the surgeon about the onset of colds or sore throat, cough or skin diseases. Fasting from midnight of the day prior to surgery. It is also necessary to arrange with someone for their presence throughout the post-operative period.
Surgical procedure
Depending on the chronology of the surgical approach and the technique used, we can distinguish between open and close rhinoplasty , or partial or complete rhinoseptoplasty. "Primary Rhinoplasty" is when surgery is performed for the first time, "Secondary or Revision Rhinoplasty" when the patient's nose has been already operated on. The latter type of nose job is designed to fix any residual defects or defects that result from previous nose surgery. A nose job can be approached using either a closed or open technique. "Closed" rhinoplasty is normally used for a nose that has never undergone operations or trauma, with minor defects or not particularly serious deviations. In this case the incisions are made within the inside of the nose and the scars are invisible. "Open" rhinoplasty is used to correct major defects of the tip, above all in noses that have already undergone surgery or in post-traumatic noses . In the "open" rhinoplasty, internal incisions are associated to a small incision across the columella (the section that separates the two nostrils); this scar is usually invisible. Rhinoplasty allows to reduce the size of the nose by reshaping the tip, removing osteocartilagineous humps and correcting the nose-labial angle. Not infrequently, it may be necessary to add tissue instead of removing it, particularly cartilagineous tissue. The latter is usually taken from the nasal septum cartilage or, if not available, from the cartilage of the ear or rib. The cartilage taken will be modeled in order to obtain various shapes of grafts that will be placed in various locations as needed (between the triangular cartilages and septum, between the wing cartilages above the back, etc.). In these cases it is always suggestible to use the "open" technique as it allows a greater vision and precision when it comes to fixing the grafts. When nostrils are too wide, it is possible to reduce their size by means of incisions at the base of the nose.
Postoperative treatment
After surgery a splint or Pinstripe made from thermolabile material is applied to keep the new shape of bones and cartilage. Usually, but not always, two small nasal gauze packings are placed and left in place for 24 hours. If septal surgery is to be performed, the gauze packings are inserted and two thin silicone strips are positioned to the sides of the septum to keep it in line and avoid any risk of hematoma. The splint is left in place for 7 to 10 days. Rhinoplasty is not a painful operation and anyway, if some pain is felt, it can be easily treated with common analgesics.
In the early days after surgery, some bruising and swelling normally appear around the eyes: they will disappear within 8 to 10 days. It is advisable to keep the head raised during the first two days after surgery and avoid any physical effort. There are a few things that must absolutely be avoided after a nose job: exposure to direct sun, saunas, Turkish baths, taking very hot food and drinks.
After removal of the splint, patches will be applied on the back of the nose for several days in order to minimize swelling. The use of glasses should be avoided for at least a month. The aesthetic result, already visible after the first two weeks, will be definitely achieved after 6 to 12 months after surgery, as all throughout this period swelling progressively reduces and the nose takes the desired shape.
Possible risks and complications
Some minor complications may occur (bleeding, hematoma, localized infection, dehiscence of sutures, intolerance to suture materials and dressing) as in any surgery. The scars are located inside the nose and are thus virtually invisible: if nostrils are too wide or an open Rhinoplasty has been performed, the scars are visible. Like all scars, they can be subject to hyper/hypopigmentation, or hyper/ hypotrophy at varying degrees depending on the genetic characteristics of each patient; this event is unpredictable. The scars that grow internally can also be exuberant and in some cases can cause, especially close to the tip, bulges (supratip) which can be difficult to treat. If synthetic materials are used, instead of cartilage grafts, some intolerance may emerge which will show at varying degrees ranging from mere redness of the skin until sores and spontaneous extrusion of the implant; should this be the case, then the implanted material will have to be removed. Some asymmetry may occur due to abnormal scarring or bony or cartilaginous residues, formation of exuberant bone callus, absorption or displacement of cartilaginous grafts.
In these cases, when the surgeon judges it fit, a light revision surgery is performed usually in local anesthesia.
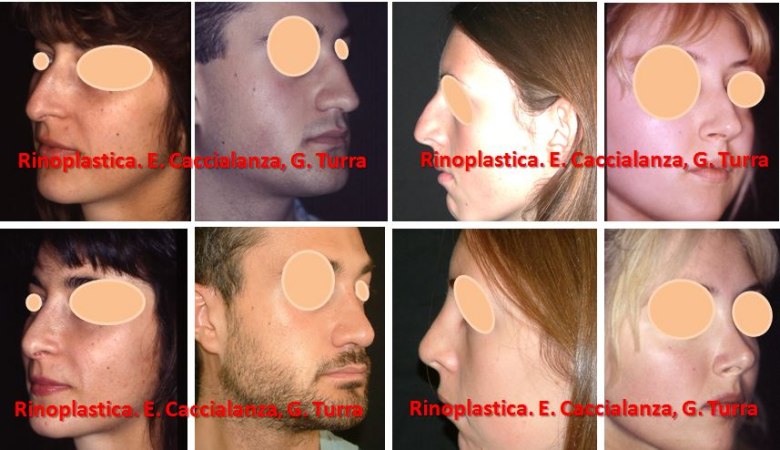
| BEFORE AND AFTER |
|
|
|



















